Kidney Stones
Expert evaluation, treatment, and prevention — helping you get relief and reduce your risk of recurrence.
Kidney stones are hard mineral deposits that form inside the kidneys when substances in the urine — such as calcium, oxalate, and uric acid — become too concentrated and crystallize. They affect roughly 1 in 10 Americans, and rates have been rising over the past several decades. Stones range from a grain of sand to larger than a marble, and they can cause excruciating pain when they move from the kidney into the ureter, the narrow tube that carries urine to the bladder.
Most people experience their first stone between ages 40 and 60, and men are affected more often than women (about 11% vs. 7%). If you have had one stone, you have approximately a 50% chance of forming another within five years without preventive measures — which is why evaluation and long-term prevention are just as important as treating the stone itself.
Types of Kidney Stones
Knowing which type of stone you have helps guide both treatment and prevention.

Calcium Oxalate
70–80% of stonesForm when calcium combines with oxalate in the urine. Contrary to popular belief, restricting calcium is usually not the answer — in fact, too little dietary calcium can increase your risk.
Uric Acid
5–10% of stonesMore common in people with gout, diabetes, or diets very high in animal protein. They form in acidic urine and can often be prevented or even dissolved by making the urine more alkaline.
Struvite
Infection stonesCaused by chronic urinary tract infections. Certain bacteria produce ammonia that raises urine pH, encouraging the growth of large, branching stones that can fill the entire kidney.
Cystine
Rarest typeCaused by an inherited condition called cystinuria. These stones tend to form at a young age and require specialized, lifelong management.
A stone sitting quietly in the kidney may cause no symptoms at all. Pain typically begins when a stone enters the ureter and obstructs urine flow, causing the kidney to swell and the ureter to spasm.
- Severe, sudden flank pain — in the side and back below the ribs, often radiating to the lower abdomen and groin. This pain comes in intense waves and is widely described as one of the most painful experiences a person can have.
- Blood in the urine (hematuria) — urine may appear pink, red, or brown.
- Nausea and vomiting — common during acute episodes due to shared nerve pathways between the kidney and the stomach.
- Urinary urgency, frequency, or burning — especially as the stone nears the bladder.
- Fever and chills — signal a possible urinary tract infection alongside the stone, a serious combination that requires immediate medical attention.
- Dehydration is the single most common cause. When you don't drink enough fluids, your urine becomes concentrated, allowing minerals to crystallize more easily.
- Diet plays a major role. High sodium intake forces more calcium into the urine. Diets very high in animal protein increase uric acid and reduce citrate, a natural stone inhibitor.
- Family and personal history — if a parent or sibling has had stones, your risk is significantly higher. A prior stone roughly doubles your lifetime risk.
- Obesity and metabolic syndrome — higher BMI, diabetes, and hypertension are all independently associated with stone formation.
- Certain medical conditions such as hyperparathyroidism, inflammatory bowel disease, chronic UTIs, and gout can predispose to stones.
When a kidney stone is suspected, a non-contrast CT scan is the gold standard for diagnosis. It quickly identifies the stone's size, location, and number with high accuracy, and it does not require contrast dye. A CT scan also helps rule out other causes of abdominal pain.
A urinalysis checks for blood in the urine, signs of infection, and urine pH. Blood work evaluates kidney function, calcium levels, and uric acid. Together, these results help Dr. Radtke determine whether the stone is likely to pass on its own or whether intervention is needed.
If you have passed a stone, stone analysis — sending the stone to a laboratory — reveals its exact composition and is invaluable for guiding prevention. Always strain your urine and save any stone fragments you pass.
Whether a stone can pass without surgery depends primarily on its size and location:
Stones 4 mm or smaller have a very high chance of passing spontaneously — most will pass within days to a few weeks with hydration and pain management.
Stones 5–10 mm have a moderate chance of passing, especially if located in the lower (distal) ureter near the bladder. A medication called tamsulosin (an alpha-blocker) can relax the ureter and significantly improve the odds of passage. This is called medical expulsive therapy and is typically tried for up to 4–6 weeks.
Stones larger than 10 mm rarely pass on their own and usually require a procedure.
Other factors also matter: stones that have not moved after several weeks, stones causing persistent pain or vomiting, stones blocking a kidney with signs of infection, or stones in patients with a solitary kidney all warrant early intervention. Dr. Radtke will discuss the options and timeline with you so you can make an informed decision about waiting versus proceeding with treatment.
Treatment Options
The right approach depends on stone size, location, composition, and your anatomy. Dr. Radtke will recommend the most effective option for your situation based on current American Urological Association guidelines.
Medical Expulsive Therapy
For ureteral stones 10 mm or smaller that have a reasonable chance of passing, treatment focuses on pain control (anti-inflammatories and, when needed, stronger medications), generous hydration, and an alpha-blocker such as tamsulosin to relax the ureter and speed passage. Close follow-up with imaging ensures the stone is progressing and the kidney is not at risk.
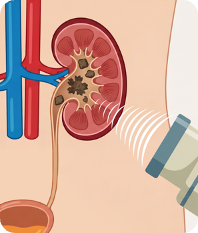
Shock Wave Lithotripsy (SWL)
Focused sound waves from outside the body break the stone into small fragments that can pass in the urine. SWL is noninvasive — no incisions or scopes — and is performed as an outpatient procedure under sedation. It works best for kidney stones up to about 2 cm (and up to 1 cm for lower-pole stones) and smaller ureteral stones. Multiple sessions may occasionally be needed.
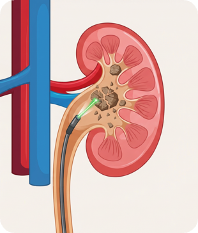
Ureteroscopy with Laser Lithotripsy
A thin, flexible scope is passed through the urethra, bladder, and up into the ureter or kidney — no external incisions. Once the stone is located, a laser (holmium or thulium fiber) fragments it into tiny pieces that are removed with a basket or reduced to dust. Ureteroscopy offers higher stone-free rates than SWL and is effective for stones of all compositions and most sizes throughout the urinary tract.
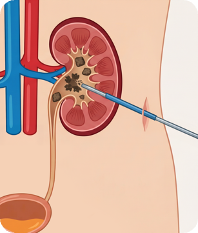
Percutaneous Nephrolithotomy (PCNL)
For large kidney stones (generally >2 cm) or complex stone burdens such as staghorn calculi, PCNL is the recommended first-line treatment. A small incision in the back provides direct access to the kidney, allowing the stone to be broken up and removed through a scope. PCNL achieves the highest stone-free rates for large stones and is performed under general anesthesia with a short hospital stay.
Because the recurrence rate for kidney stones can reach 50% within five years, prevention is a critical part of stone care. Dr. Radtke provides a thorough approach to reduce your risk of future stones.
Hydration
Increasing fluid intake is the single most effective prevention strategy. The goal is to produce at least 2.5 liters of urine per day — enough that your urine stays light yellow or clear. Water is ideal.
Adequate hydration alone can reduce stone recurrence by up to 50%.
Dietary Modifications
- Reduce sodium — aim for less than 2,300 mg per day. High salt forces more calcium into the urine.
- Get enough calcium from food — dietary calcium actually reduces stone risk by binding oxalate in the gut. Aim for 1,000–1,200 mg daily.
- Moderate animal protein — excess red meat, poultry, and seafood increase uric acid and lower citrate.
- Limit high-oxalate foods — spinach, rhubarb, beets, nuts, and chocolate. Pair these with calcium-rich foods to reduce absorption.
24-Hour Urine Metabolic Workup
For recurrent stone formers, Dr. Radtke recommends a 24-hour urine collection that measures volume, calcium, oxalate, citrate, uric acid, sodium, and pH. This identifies the specific metabolic abnormalities driving your stone formation and guides targeted treatment.
Only 7–16% of stone patients undergo this evaluation — a gap Dr. Radtke works to close.
Medications for Prevention
When dietary changes alone are not enough, medications can significantly reduce recurrence:
- Thiazide diuretics — lower urine calcium
- Potassium citrate — raises urine citrate and pH
- Allopurinol — lowers uric acid
The right medication is chosen based on your 24-hour urine results and stone type.
Most kidney stones, while painful, can be managed in the outpatient setting. However, certain situations require immediate emergency care:
- Fever or chills with a known or suspected stone — suggests an infected, obstructed kidney that can rapidly progress to sepsis.
- Severe pain that cannot be controlled with over-the-counter or prescribed pain medications.
- Persistent nausea and vomiting that prevent you from keeping down fluids or medications.
- Inability to urinate or a significant decrease in urine output.
- Stone in a solitary kidney — if your only functioning kidney becomes obstructed, prompt intervention is essential.
If you are experiencing manageable pain and have no signs of infection, a scheduled appointment with Dr. Radtke is appropriate. He will evaluate your stone, discuss your options, and develop a plan.
Get Help with Kidney Stones
Schedule a consultation with Dr. Radtke for evaluation and treatment.
Schedule an Appointment
Dr. Radtke sees patients through Prevea Health. You can book an appointment online or call our office directly.
Clinic Information
(920) 458-6664
Monday – Friday: 8:00 AM – 5:00 PM
Saturday – Sunday: Closed